Metals and the Brain: The Role of Heavy Metal Exposure in Parkinson’s Risk
Many people want to understand how long-term environmental exposure affects the brain. Parkinson’s disease has many influences, and the picture is complex.
![How-Heavy-Metals-Like-Lead-and-Mercury-May-Fuel-Parkinsons-Photo-1 | The Parkinson's Plan | The Parkinson's Plan Crumbled aluminum foil pieces floating in a clear liquid, reflecting light from all sides.] ,](https://theparkinsonsplan.com/wp-content/uploads/2026/04/How-Heavy-Metals-Like-Lead-and-Mercury-May-Fuel-Parkinsons-Photo-1-1024x492.png)
Research continues to point to heavy metals as an important area of study. People often ask whether exposure to metals like manganese or lead affects neurological health, and why some communities face higher rates of neurological conditions.
Our goal is to provide clarity, not medical direction. As science evolves, we help people understand what is known, what is emerging, and why heavy metal exposure has become a meaningful part of the conversation around Parkinson’s causes and long-term neurobiology.
Why Heavy Metals Are On The Radar Of Parkinson’s Researchers
Heavy metals such as manganese, lead, mercury, and others, are naturally occurring elements, but industrialization has dramatically increased human exposure. When these metals accumulate in the body, especially over long periods, they can affect cellular energy production, oxidative balance, and inflammatory pathways. These pathways overlap with mechanisms currently being studied in Parkinson’s research.
Although heavy metals are not considered direct causes of Parkinson’s, researchers have noticed associations between prolonged exposure and neurological patterns relevant to the condition. As environmental monitoring becomes more precise, the scientific community has started examining how chronic exposure may influence the brain’s vulnerability.
Manganese: A Metal With A Longstanding Connection To Movement Disorders
Among the metals studied in relation to Parkinson’s, manganese has the longest documented relationship with motor dysfunction. This connection is particularly evident in occupational settings such as welding, mining, and ferroalloy production, where workers may inhale manganese-containing particulates over many years.
What the Research Tells Us:
● THE “WELDERS STUDY”: A landmark study by researchers at Washington University School of Medicine found that welders exposed to manganese levels below current federal safety limits still exhibited neurological symptoms similar to Parkinson’s. This suggests that even “allowable” levels of exposure can influence brain health over time.
● DOPAMINE MARKER REDUCTIONS: Research funded by the Michael J. Fox Foundation used PET scans to show that long-term manganese exposure in industrial workers led to an 11.7% reduction in dopamine markers in the caudate, a key structure in the brain’s movement center.
● THE “MANGANISM” DISTINCTION: High-level exposure can lead to a condition known as manganism. While it presents symptoms like tremors and stiffness that look like Parkinson’s, a 2025 review in Frontiers in Pharmacology notes a key biological difference: whereas Parkinson’s primarily involves the loss of dopamine-producing neurons, manganese exposure may instead cause those neurons to become dysfunctional, preventing the effective release of the dopamine they still hold.
Researchers distinguish manganism from Parkinson’s clinically, notably, manganism often does not respond to traditional L-dopa treatments, but the biological overlap makes it an essential topic. Both conditions involve oxidative stress and mitochondrial strain, which is why manganese remains a cornerstone of environmental neurotoxicology.
At The Parkinson’s Plan, we view manganese as a “biological mirror.” It helps us understand how environmental factors can intersect with neurological pathways, providing a clearer map of how we might protect our brains from long-term cumulative stress.
Lead Exposure And Its Long-Term Effects
Lead is a “legacy” metal, meaning it often remains in the human body long after the initial exposure has ceased. Historically used in paint, gasoline, pipes, and industrial manufacturing, lead exposure has impacted numerous communities, often disproportionately affecting older urban infrastructure and underserved areas.
The “Bone Reservoir” Effect
Unlike some toxins that are filtered out quickly, 90% to 95% of lead in adults is stored in the bones.
● Long-Term Release: Lead mimics calcium, allowing it to integrate into the bone matrix. It can stay there for 20 to 30 years.
● The Internal Exposure Loop: As we age, or during periods of bone density loss (like menopause or certain illnesses), this stored lead is released back into the bloodstream. This creates a “second wave” of exposure, meaning the brain can be affected by lead that was inhaled or ingested decades prior.


How Lead Impacts Neurological Resilience
While lead is rarely the sole cause of Parkinson’s, it acts as a biological stressor in three key ways:
1. Mitochondrial “Suffocation”: Lead interferes with how cells produce energy. Since the neurons responsible for movement are some of the most energy-hungry cells in the body, they are particularly vulnerable to this disruption.
2. The Calcium Imposter: Because lead mimics calcium, it can “trick” the brain’s signaling system, causing neurotransmitters to fire incorrectly or at the wrong times, leading to cellular exhaustion.
3. Chronic Neuroinflammation: Even low levels of lead can keep the brain’s immune cells (microglia) in a state of “high alert.” Over years, this low-grade inflammation can damage the very neurons that Parkinson’s research focuses on.
Environmental Justice And Health Equity
At The Parkinson’s Plan, we believe it is vital to acknowledge that lead exposure is not distributed equally. Because of historical housing policies and industrial zoning, individuals in older, underserved neighborhoods often carry a higher “body burden” of lead. Understanding this link is an essential step in advocating for both community health and personalized neurological care.
Mercury: A Potent Neurotoxin And The Brain
Mercury is a naturally occurring metal, but industrial activities have significantly increased human exposure. Unlike lead, which settles in the bones, mercury has a high affinity for fatty tissues, making the brain a primary target for accumulation.
The Blood-Brain Barrier And Methylmercury
The most concerning form of mercury is methylmercury. It is uniquely dangerous because it mimics essential amino acids, tricking the blood-brain barrier into allowing it entry into the central nervous system.
Once inside, mercury is difficult to remove. It concentrates in the cerebellum and the basal ganglia, the specific brain regions responsible for coordinating smooth, purposeful movement.
Mechanisms Of Neurological Damage
Mercury disrupts the internal machinery of neurons through three primary pathways.
● Microtubule Collapse Neurons rely on microtubules to transport nutrients and signals. Mercury binds to these structures, causing them to collapse and essentially cutting off the cell’s internal supply chain.
● Antioxidant Depletion Mercury binds to glutathione, the brain’s primary defense against oxidative stress. By depleting this protector, mercury leaves dopaminergic neurons vulnerable to metabolic damage.
● Glutamate Excitotoxicity Mercury prevents the brain from regulating glutamate. High levels of this neurotransmitter overstimulate neurons to the point of exhaustion and death, a process observed in various neurodegenerative conditions.
Sources And Agency
Exposure typically occurs through industrial emissions or the consumption of large, long-lived predatory fish. At The Parkinson’s Plan, we view mercury as a factor where individuals have agency; informed dietary and environmental choices can actively reduce your cumulative toxic load.
Common Biological Themes In Metal Exposure And Parkinson’s
While each metal has a unique “fingerprint,” they all converge on several biological themes that are central to Parkinson’s research. By understanding these commonalities, we can see why environmental monitoring is so vital to long-term brain health.
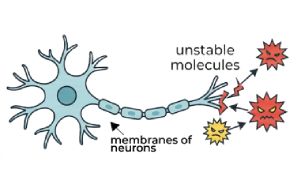
OXIDATIVE STRESS
Metals act as catalysts that create unstable molecules, damaging the protective membranes of neurons.

MITOCHONDRIAL STRAIN
By disrupting cellular energy production, metals make it harder for neurons to repair themselves.
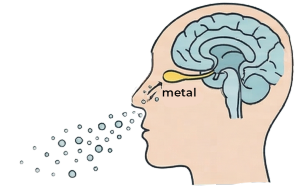
THE OLFACTORY GATEWAY
Many metals enter the body through the olfactory system (the nose), the same pathway researchers study for the very earliest signs of neurological change.
Go Deeper: New Book Coming Summer 2026
Upcoming book, Toxic Tremors: What You Haven’t Been Told About Parkinson’s (Summer 2026), reveals how environmental chemicals contribute to Parkinson’s disease and what you can do about it.
Where Heavy Metal Exposure Typically Occurs
Exposure is rarely the result of a single event; it is often the cumulative result of where we live, work, and grow. Because these elements are often invisible, identifying potential sources is the first step toward proactive health management.
● Residential Environments Older homes and urban infrastructure are the most common sources of “legacy” exposure. This includes residual lead-based paints, aging plumbing systems with lead pipes or solder, and contaminated soil in yards where industrial runoff once occurred.
● Occupational Settings Certain industries involve long-term contact with metallic dust or fumes. Workers in welding, mining, battery manufacturing, and industrial painting may inhale fine particulates daily, allowing metals to enter the bloodstream through the respiratory system.
● Community and Geography Proximity to industrial hubs, power plants, or smelting facilities can increase exposure to airborne particulates. In some regions, naturally occurring geological deposits can also leach metals into local well water or agricultural soil.


Environmental Awareness As A Path To Empowerment
While heavy metals are not direct causes of Parkinson’s, the research reinforces a critical principle: long-term exposure to environmental toxins can influence the brain’s resilience over decades. This perspective doesn’t replace what we know about genetics or aging; it simply adds a vital layer to the multi-dimensional framework of neurological risk.
At The Parkinson’s Plan, we believe that understanding these factors is not about fostering fear, but about providing clarity. No single environmental change can “prevent” the disease, but shifting from passive exposure to active awareness gives you agency. By understanding what is in your air, water, and workplace, you gain the power to:
● Advocate for safer community and occupational conditions.
● Improve your immediate household environment.
● Approach long-term wellness with the confidence that comes from balanced education.
Frequently Asked Questions
Research shows associations between long-term heavy metal exposure and neurological patterns relevant to Parkinson’s, though metals are not considered direct causes.
High-level manganese exposure has been associated with movement disorders and is frequently studied due to its overlap with dopaminergic pathways.
Some studies suggest a relationship between cumulative lead exposure and neurological vulnerability, making it a continuing area of scientific interest.
They can contribute to oxidative stress, mitochondrial dysfunction, and inflammation, mechanisms also studied in Parkinson’s research.
Because neurological health develops across decades, researchers examine how long-term environmental exposures may interact with biology and aging.